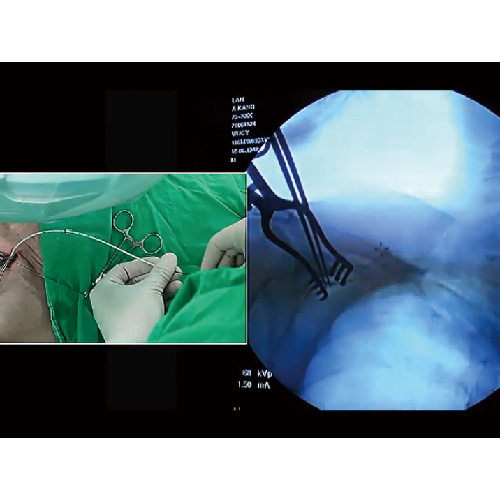
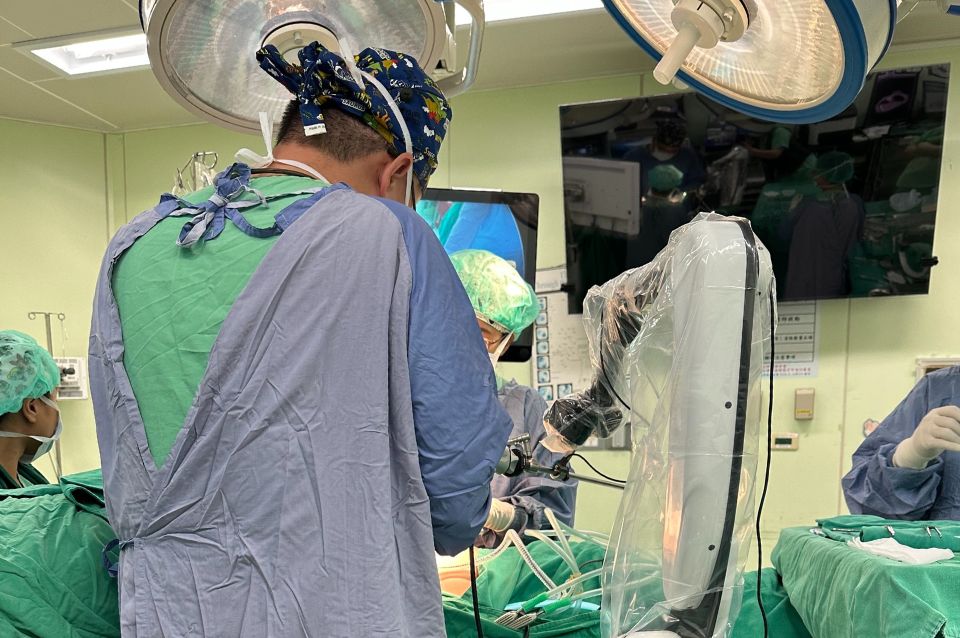
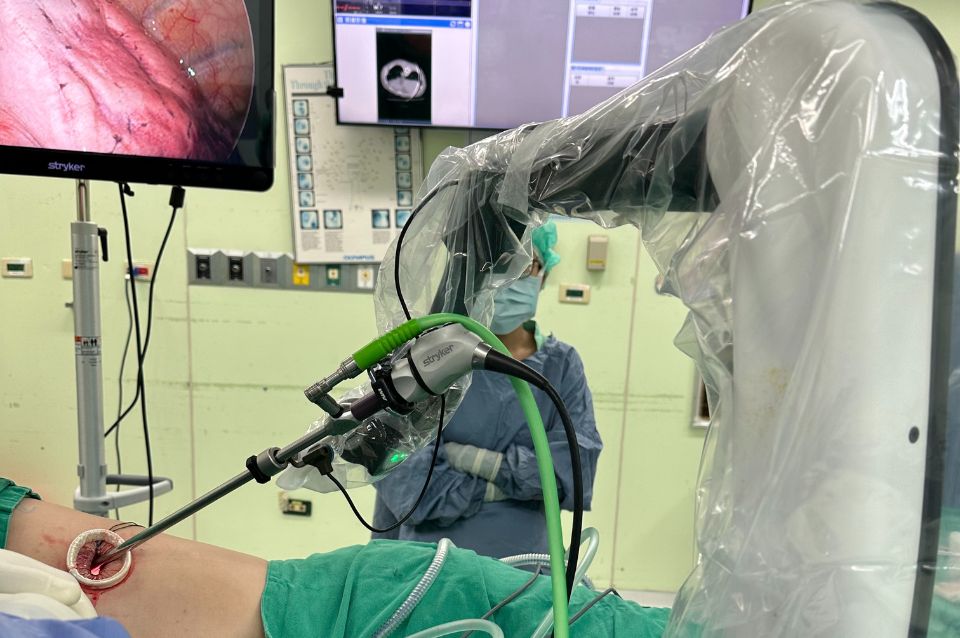
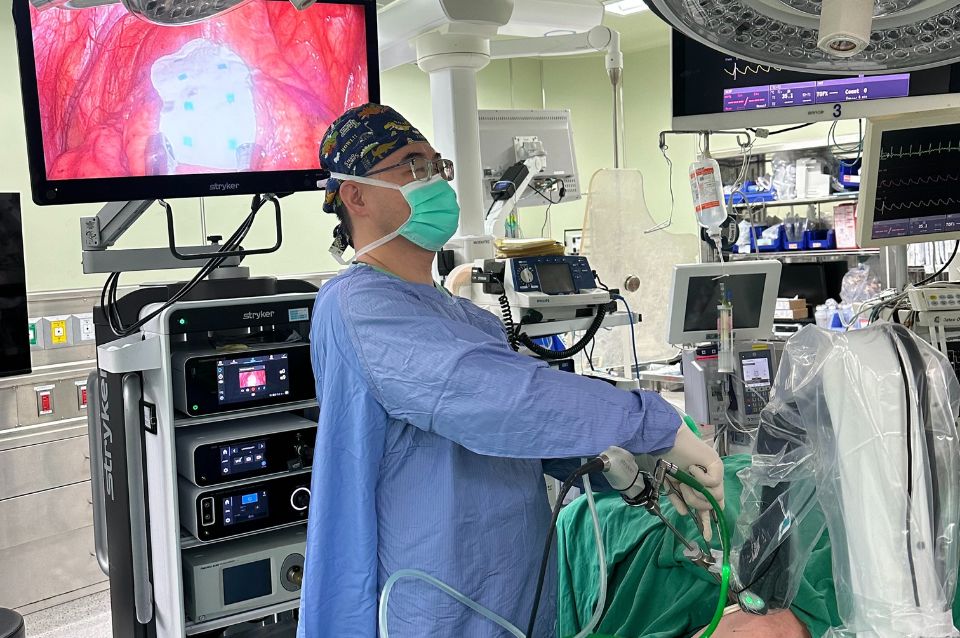
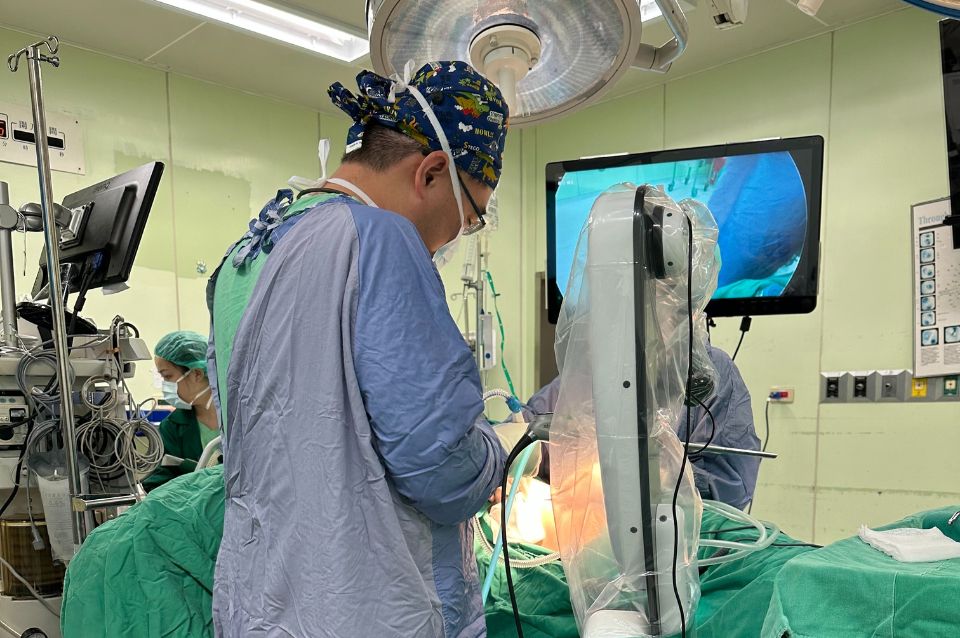
Port-A Catheter: Key Facts
- Chemotherapy drugs can damage veins, making peripheral veins unsafe.
- A Port-A catheter provides a reliable access point for repeated injections.
- Removal is considered 1-2 years after chemo if no recurrence occurs.
- Ports can be used for blood tests but require special needles and flushing.
- High-pressure ports allow contrast injections for better imaging.
What Is a Port-A?
A Port-A catheter, also called an artificial blood vessel, replaces veins for repeated treatment access.
Indications for Port-A Catheter
1. Cancer patients on chemo or immunotherapy
2. Patients requiring long-term IV nutrition
3. Blood disorder patients needing transfusions
4. Long-term use of strong medications
Port-A Surgery: Pre-Op Notes
1. 30-minute outpatient procedure, no hospitalization.
2. Inform the doctor if on blood thinners, have clotting issues, arrhythmia, or a pacemaker.
3. No fasting needed; take regular meds except blood thinners.
Local vs. General Anesthesia
Most patients need only local anesthesia for pain control. General anesthesia is required for those with neurological surgery history, epilepsy, or permanent tracheostomy with excessive secretions.
Postoperative Care
The port can be used immediately if needed, as the injection site is covered by normal skin.
No special wound care is required, but keep the area dry for a week. Avoid shoulder rotation and stretching movements, such as yoga.
Contraindications
Port-A implantation has no absolute contraindications but requires adjustments in certain conditions:
1. Bleeding disorders
2. Regular use of blood thinners (may require temporary discontinuation)
3. Implanted pacemaker (needs mode adjustment by the manufacturer)
Potential Complications
Reoperation is needed if the following occur, though the risk is only 1-2% with standard implantation:
1. Catheter or skin flap infection
2. Catheter displacement
3. Deep vein thrombosis
4. Catheter fracture
Port-A SurgerySee Dr. Wu
Specialized Excellence
Prevent Pneumo/Hemothorax
Use native veins first, ultrasound if needed.

Preserve Native Veins
Avoid internal jugular puncture with venography.
Vascular Assessment
Determine optimal access route.
Shorter Surgery
Use CT/ultrasound to check veins.
Quality Monitoring
X-ray confirms catheter position and connection integrity.
Thoracic Surgeon
DR. CHING-YANG WU
Dr. Wu summarized clinical experience to identify risk factors for Port-A complications and developed a standardized implantation protocol based on research and patient outcomes.
About DR. CHING-YANG WU
- Thoracic Surgeon, Linkou Chang Gung
- Associate Professor, Chang Gung University
- Associate Professor, Chang Gung Hospital
- Instructor, Thoracic & Cardiovascular Surgery Association
- Instructor, Thoracic Surgery Association

Thoracic Booking
Chang GungTaoyuan
- Address:No. 123, Dinghu Rd., Guishan Dist., Taoyuan City
- Call to Book:03-3196200
- Clinic Hours:Thu. 8:30 AM – 12:00 PM
- Book Now:Taoyuan Chang Gung Thoracic Surgery
Chang GungLinkou
- Address:No. 5, Fuxing St., Guishan Dist., Taoyuan City
- Call to Book:03-3281200
- Clinic Hours:Fri. 1:00 PM – 5:00 PM
- Book Now:Linkou Chang Gung Thoracic Surgery
Port-A SurgerySee Dr. Wu
Port-A Implantation Steps
-
 1
1Assessment
Evaluate condition and vein access
-
 2
2Incision and Access
Apply anesthesia, make a small cut, locate the vessel
-
 3
3Placement
Insert catheter, confirm position via X-ray
-
 4
4Fixation
Connect and secure the port under the muscle
-
 5
5Closure
Suture the incision to complete the procedure

Port-A FAQ
How Long Does a Port-A Last?
A Port-A catheter is typically kept for 2-3 years, until treatment is complete and follow-up confirms no recurrence.
Made from biocompatible materials (polyurethane, silicone, titanium), it generally does not trigger immune reactions but may degrade over time due to material fatigue.
When Should a Port-A Be Removed?
1. Complications: Immediate removal if infection, displacement, thrombosis, or catheter fracture occurs.
2. After Treatment:
‧For post-surgery cancer patients, removal is considered after 1-2 years of stable follow-up (total placement ~2-3 years).
‧For those on long-term systemic therapy (chemo, immunotherapy, targeted therapy), removal depends on tumor control and oncologist evaluation.
How Often Should a Port-A Be Flushed?
A Port-A is a closed system that must be flushed after each use to prevent residue buildup.
During treatment breaks, it is typically flushed every 3 months during oncology follow-ups.
Does a Port-A Contain Metal?
Yes, the injection port may have a titanium base, but all materials are highly biocompatible and do not cause adverse reactions.
How Much Does a Port-A Cost?
Some models are covered by National Health Insurance (NHI), making the cost fully reimbursed for eligible patients.
Does Getting a Port-A Hurt?
Local anesthesia is used during the procedure, causing brief discomfort when injected.
Once numb, there is no pain, but sensations of pressure remain.
After anesthesia wears off (1-2 hours), patients may feel tightness or a foreign body sensation, which typically fades within 2-3 days.
What If a Port-A Gets Infected?
If infection occurs, the port may need to be removed.
After 7-10 days of antibiotic treatment, a new port can be placed once the infection is under control.
Port-A SurgerySee Dr. Wu
PressCoverage
 Health LTN
Health LTN
Advancing Large-Cell Lung Cancer Treatment: NCYU & Chang Gung Memorial Hospital, Linkou Collaborate
Associate Professor of NCYU and Dr. Wu’s team collaborate on large-cell lung cancer research, yielding significant findings...
Dr. Wu Receives AATS Graham Award at ASCVTS 2016
Dr. Wu excelled in the AATS Graham Award evaluation, delivering his research within the 12-minute limit (10-minute presentation + 2-minute Q&A)...

Dr. Wu’s Team Publishes Study on Three CT-Guided Techniques for Lung Lesion Localization in the European Journal of Radiology!
From September 2019 to August 2021, the team analyzed 418 patients with lung lesions, comparing three CT-guided...

Dr. Wu’s Team Publishes Study on 3D Simulation Training for Oncology Nurses in Seminars in Oncology Nursing!
Since implantable venous catheters are not visible to the naked eye and can only be identified by touch, improper handling may occur...

Dr. Wu’s Research on Implantable Venous Ports Published in Medicine!
Based on literature and clinical experience, Dr. Wu formulated a standard algorithm to evaluate the best entry vessel for...

Dr. Wu’s Lung Cancer Research Published in Medicine!
Many patients still experience recurrent non-small cell lung cancer (NSCLC). To investigate, Dr. Wu and his team reviewed data from 356 stage I lung cancer patients (2005–2011), finding...

Dr. Wu’s Team Publishes Prognostic Study on Lung Adenocarcinomas ≤2cm in the Journal of the Formosan Medical Association!
The study aims to identify unique prognostic factors with clinical significance. Retrospective analysis of cases from...

Dr. Wu’s Team Publishes Study on Postoperative Circulating Tumor Cells as a Predictor of Lung Cancer Recurrence in Diagnostics!
With extensive experience in lung cancer surgery, Dr. Wu’s team investigated whether changes in circulating tumor cells (CTC)...

Dr. Wu’s Study on Central Venous Catheter Tip Placement Published in Medicine!
After analyzing 346 cases, Dr. Wu found that 221 cases (63.9%) were in the non-migration group, 67 cases (19.4%)...

Dr. Wu’s Research on a New Implantable Injection Port Published in Journal of Biomedical Materials Research Part B: Applied Biomaterials!
With in-depth studies and extensive clinical experience in implantable intravenous ports, Dr. Wu has explored complications...

Dr. Wu’s Expertise
- 2011 Taiwan Thoracic & Cardiovascular Surgery New Scholar Award
- 2012 Taiwan Thoracic & Cardiovascular Surgery President’s Award
- 2014 Taiwan Vascular Surgery Smart Award
- 2015 Taiwan Vascular Surgery Smart Award
- 2016 AATS Graham Award
- 2020 Taiwan Thoracic & Critical Care Medicine Best Paper
- 2021 Taiwan Thoracic & Cardiovascular Surgery President’s Award
- 2023 Global Injection Port Consensus Conference
InfoVideo
What Is a Port-A?
Port-A types can be classified by catheter material, high-pressure compatibility, and injection port material. Catheters are mainly made of silicone…

Why Get a Port-A?
A brief overview of the reasons for Port-A placement…

What Is a High-Pressure Port-A?
An overview of high-pressure Port-A and its clinical benefits…

How Do Healthcare Providers Use a High-Pressure Port-A?
Identification and injection procedure for high-pressure Port-A…

Post-Op Care for Port-A
Daily activities remain unrestricted, but certain movements depend on port placement…

Port-A Placement: What to Expect
An implantable venous port, commonly known as a Port-A, serves as a reliable IV access for clinical treatments. It functions like an invisible socket placed under the skin, allowing injection needles—like…